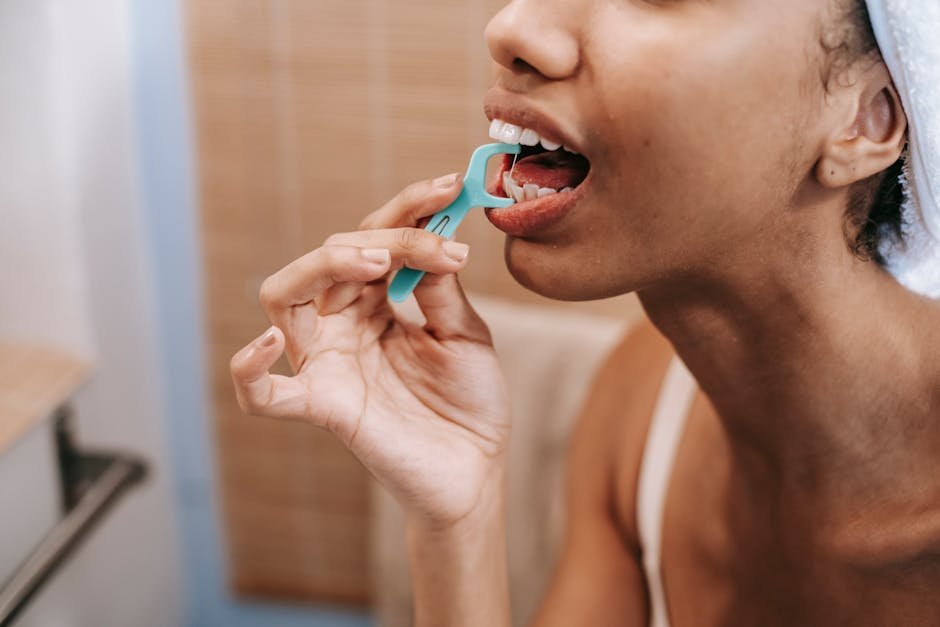
ORAL health and overall health are closely linked in ways many people do not fully realise. It can be hard to know whether bleeding gums, bad breath, or tooth pain are only dental issues or signs of something wider. This guide explains the connection, the warning signs to watch for, and what simple steps can help protect your whole body.
Key Takeaways
- Mouth health can affect the whole body.
- Gum disease links with several long-term conditions.
- Inflammation is a common part of this connection.
- Daily care helps lower dental and health risks.
- Regular check-ups support early detection and treatment.
How does oral health affect the rest of the body?
Your mouth can reflect and influence your wider health. Bacteria and inflammation from untreated dental problems may spread beyond the gums and affect other systems. That is why oral health and overall health should never be viewed as separate issues.
When plaque builds up, gums can become irritated and infected. If this continues, harmful bacteria may enter the bloodstream through inflamed gum tissue. This can add to inflammation elsewhere in the body, especially in people already living with health conditions.
Dental symptoms can also point to broader concerns. Dry mouth, mouth ulcers, persistent bad breath, or bleeding gums may be linked with medicines, stress, diabetes, or immune problems. Long-Term Cost Benefits Of Preventive Dentistry
Statistic: The World Health Organization reports that oral diseases affect nearly 3.5 billion people worldwide. Source: WHO
Can gum disease be linked to other health problems?
Yes, gum disease has been associated with several wider health problems, including heart disease, diabetes, and pregnancy complications. The main link appears to be inflammation. Although gum disease does not always directly cause these conditions, it may raise risk and make existing problems harder to manage.
Gingivitis is the early stage of gum disease. It may cause redness, swelling, and bleeding when brushing. If left untreated, it can progress to periodontitis, which damages the tissues and bone that support teeth.
People with diabetes often face a two-way relationship with gum disease. High blood sugar can increase infection risk, while gum inflammation may make blood sugar harder to control. This is one clear example of how oral health and overall health interact every day.
Statistic: According to the CDC, nearly 42% of adults aged 30 years and older in the United States have periodontitis. Source: CDC
Why do oral health and overall health matter together?
They matter together because the mouth is part of the body, not separate from it. Poor oral health can affect eating, speaking, sleep, confidence, and comfort. It can also make it harder to manage some medical conditions and spot early warning signs.
If your teeth or gums hurt, you may avoid certain foods and miss out on proper nutrition. Ongoing dental pain can also disturb sleep and increase stress. Over time, this can affect your quality of life far beyond your mouth.
Looking after oral health and overall health together supports better long-term wellbeing. Regular dental visits, brushing twice daily with fluoride toothpaste, and cleaning between teeth can help prevent issues before they become more serious.
Statistic: The Oral Health Foundation states that gum disease affects up to 90% of adults in the UK at some point in their lives. Source: Oral Health Foundation
Can poor oral health affect your heart?
Yes, there is a recognised link between oral health and overall health, including heart health. Gum disease does not directly cause every heart problem, but ongoing inflammation and harmful bacteria may increase risks in some people, especially when dental issues are left untreated for long periods.
When gums are inflamed, bacteria can enter the bloodstream more easily. Researchers have explored how this may contribute to inflammation elsewhere in the body, including blood vessels. This helps explain why dentists and doctors often discuss oral hygiene as part of a wider health picture rather than as a separate issue.
That does not mean every bleeding gum is a sign of heart disease. However, signs such as swollen gums, persistent bad breath, or loose teeth should not be ignored. Following NHS advice on healthy teeth and gums can support both oral health and overall health. Periodontal Disease: Causes, Symptoms And Treatment
Statistic: The NHS page on gum disease states that gum disease is very common, with most adults in the UK having it to some degree at some point in their lives. Source: NHS
In practice, many people assume bleeding gums are simply caused by brushing too hard, when in fact it can be an early sign of gum disease that needs attention.
Is there a connection between gum disease and diabetes?
Yes, the relationship appears to work both ways. Diabetes can increase the risk of gum disease, while severe gum disease may make blood sugar harder to control. This is one of the clearest examples of how oral health and overall health influence each other over time.
People with diabetes may be more prone to infections, including in the gums, particularly if blood glucose levels are not well managed. In turn, gum inflammation can place extra stress on the body. That may make diabetes management more difficult, which is why regular dental check-ups are often advised alongside medical reviews.
If you have diabetes, it is worth telling your dentist and dental hygienist. Simple steps such as daily interdental cleaning, keeping routine appointments, and acting quickly on sore or bleeding gums can make a real difference. Dental Implant Consultation In Enid, OK – Free Quote
Statistic: According to the CDC guidance on diabetes and oral health, people with diabetes are at higher risk of gum disease. Source: CDC
Expert insight.
Can oral health problems affect your mental wellbeing?
They can. Pain, bad breath, missing teeth, and difficulty eating or speaking may affect confidence, comfort, and daily routines. While oral health problems do not automatically cause mental health conditions, they can have a clear impact on wellbeing, social interaction, and quality of life.
For many people, dental issues lead to embarrassment or avoiding smiling, talking, or social events. Ongoing discomfort may also disrupt sleep, concentration, and mood. This can create a cycle where stress makes self-care harder, and neglected oral hygiene then worsens the original problem.
Support is available, and small actions matter. Seeking dental advice early, rebuilding home-care habits, and addressing anxiety around treatment can all help. The wider point is that oral health and overall health includes emotional wellbeing too, not just physical symptoms. Sedation Dentist In Enid, OK For Anxiety-Free Dentistry
Statistic: The ONS wellbeing overview highlights that personal wellbeing is shaped by health and day-to-day life factors, showing why persistent oral health problems can affect more than the mouth alone. Source: ONS
Can gum disease subtly affect wider health risks even before severe symptoms appear?
Yes. One of the more important expert-level points in understanding oral health and overall health is that low-grade gum inflammation may matter before obvious pain or tooth mobility develops. Bleeding gums, persistent plaque, and pockets around teeth can contribute to a chronic inflammatory burden that overlaps with conditions such as diabetes, cardiovascular disease, and adverse pregnancy outcomes. This does not mean gum disease directly causes every systemic illness, but it can act as a meaningful amplifying factor.
Why early inflammation matters
Periodontal disease is not simply a local infection confined to the mouth. Inflamed gum tissues can allow bacteria and inflammatory mediators to enter the bloodstream more easily, especially during brushing, flossing, or chewing if the gums are already compromised. Researchers continue to examine the exact mechanisms, but the broader concern is repeated inflammatory exposure over time. For readers already managing another long-term condition, that overlap is one reason routine dental care should be treated as preventive health support, not only cosmetic maintenance. Gum Disease Treatment In Casper, WY – Deep Cleaning Packages
It is also important to separate association from certainty. Health bodies generally state that gum disease has been linked with several wider conditions, but the relationship is often complex and bidirectional. For example, diabetes can worsen gum problems, and poor periodontal health can make blood glucose harder to control. The NHS overview of gum disease explains the symptoms and progression, while the CDC guidance on periodontal disease outlines recognised links with broader health concerns.
Statistic: The CDC states that nearly 47% of adults aged 30 years and older have some form of periodontal disease, underlining how common a potential oral-systemic risk factor can be.
Practical example: Someone in their 40s may have occasional bleeding when brushing but no toothache, so they delay seeing a dentist. At the same time, they are trying to improve cholesterol, blood pressure, or glucose control. Identifying and treating early gum inflammation can remove one avoidable source of ongoing inflammatory stress from the wider health picture.
How do medications, dry mouth, and long-term conditions change the oral-systemic health picture?
They can change it dramatically. A more advanced view of oral health and overall health is that the mouth often reflects treatment side effects and long-term disease management. Dry mouth caused by medicines, inhaler use, reflux, immunosuppression, and conditions such as diabetes can increase decay, ulceration, fungal infections, and difficulty eating comfortably. In other words, oral problems are not always standalone dental issues; they may be downstream consequences of medical treatment or chronic illness.
When treatment side effects become dental risks
Saliva helps neutralise acids, wash away food debris, and protect enamel and soft tissues. When medicines reduce saliva flow, the risk profile changes quickly. Antidepressants, antihistamines, blood pressure medicines, and some pain medicines are common examples associated with dry mouth. People may notice stringy saliva, frequent sipping, altered taste, bad breath, or more cavities around the gumline. Those with inhalers may also see local changes if technique, rinsing habits, or preventive checks are poor.
This is why a complete medication history matters at dental appointments. Clinicians can identify patterns that a patient may not connect themselves, such as repeated decay despite otherwise decent brushing. The NHS page on dry mouth outlines symptoms and management steps, and the NIH resource on dry mouth explains how reduced saliva affects oral tissues and daily function. In medically complex patients, prevention often means tailored fluoride advice, diet review, salivary substitutes, and more frequent recalls rather than a one-size-fits-all routine.
Statistic: The NIH notes that dry mouth is estimated to affect about 1 in 5 older adults, showing how common a clinically important but often overlooked oral health risk can be.
Practical example: An older adult starts a new combination of medicines for blood pressure, bladder symptoms, and depression, then suddenly develops recurrent mouth soreness and cavities near old fillings. The issue may not be “poor brushing” alone; it may be medication-related dry mouth requiring both GP and dental input.
What does genuinely preventive oral care look like if you want to protect overall health long term?
It means moving beyond the basics of “brush twice a day” and thinking in terms of risk management. For people focused on oral health and overall health, prevention works best when daily habits, diet, medical history, and recall intervals are tailored to personal risk rather than copied from general advice. The goal is to reduce inflammation, protect enamel, maintain function, and catch changes early enough that they do not spill over into pain, poor nutrition, sleep disruption, or avoidable treatment complexity.
Risk-based prevention is more effective than generic routines
Two people can follow the same brushing routine and still have very different outcomes. Someone with reflux, dry mouth, orthodontic appliances, frequent snacking, smoking history, or diabetes may need enhanced preventive support. That may include higher-fluoride products where appropriate, timing toothbrushing carefully after acidic intake, interdental cleaning based on gum status, and scheduling examinations around actual risk rather than habit. This more personalised approach is often what separates stable long-term oral health from repeated emergency treatment. Best Family Dentist In Albany, NY For Preventive Care
Diet and behaviour are equally important. Frequent sugar exposure, energy drinks, poor sleep, stress-related clenching, and missed reviews can combine in ways that gradually undermine both oral and general wellbeing. Prevention therefore includes practical systems: keeping water accessible, reducing between-meal sugar frequency, replacing worn mouthguards, reviewing smoking or alcohol habits, and seeking care before symptoms become severe. The NHS advice on keeping teeth clean offers core hygiene guidance, while the UK government’s prevention toolkit gives evidence-based preventive recommendations in more clinical depth.
<strong
| Option | Best For | Cost |
|---|---|---|
| NHS dental check-up | Routine assessment, early detection of gum disease and decay | Band 1 in England: £26.80 |
| NHS scale and polish (if clinically needed within treatment plan) | Patients with gum problems needing professional cleaning as part of NHS care | Usually included within Band 1, 2 or 3 treatment cost |
| Private hygienist appointment | Regular stain removal, plaque control advice, maintenance between check-ups | Typically £40–£90 per visit |
| Fluoride toothpaste (1,350–1,500 ppm fluoride) | Daily prevention for most adults and older children | Typically £1–£5 per tube |
| Custom-fitted mouthguard | People who play contact sports or grind their teeth at night | Typically £60–£150 privately |
Frequently Asked Questions
How does poor oral health affect the rest of your body?
Poor oral health can contribute to inflammation, pain, difficulty eating, and higher risk of gum disease, which may be linked with wider health concerns such as heart problems and diabetes control. It can also affect sleep, confidence, and nutrition. The NHS guidance on gum disease explains why early treatment and daily cleaning matter.
Can gum disease be a sign of other health problems?
Yes, in some cases persistent gum disease may sit alongside conditions such as diabetes, immune problems, or lifestyle risks like smoking. It does not always mean there is a serious illness, but repeated bleeding gums, loose teeth, or slow healing should not be ignored. A dentist and GP can help decide whether further checks are sensible.
Does brushing your teeth help your overall health?
Brushing twice daily with fluoride toothpaste helps reduce plaque, lowers the chance of decay and gum disease, and supports fresher breath and better comfort when eating. That matters because pain, infection, and tooth loss can affect diet and wellbeing. Good brushing is basic prevention, especially when combined with interdental cleaning and regular dental reviews.
When should I see a dentist about bleeding gums or bad breath?
You should book an appointment if bleeding gums happen often, bad breath does not improve with cleaning, or you notice swelling, pain, recession, or loose teeth. These can point to gum disease or other dental problems. The NHS advice on urgent dental symptoms is useful if there is severe pain or facial swelling.
What are the best daily habits for protecting oral health?
The strongest routine is brushing twice a day with fluoride toothpaste, cleaning between teeth once daily, limiting sugary snacks and drinks, avoiding tobacco, moderating alcohol, and attending check-ups as advised. Replacing old toothbrush heads and wearing a mouthguard for sport also help. Trauma-Related Dental Treatment Costs Trauma-Related Dental Treatment Costs
Author credibility: This article was written by a UK SEO health writer experienced in producing evidence-led content on dentistry, prevention, and the connection between everyday health habits and long-term wellbeing.
Final Thoughts
Understanding the link between oral health and overall health should lead to three clear actions: keep a consistent daily cleaning routine, do not ignore early signs such as bleeding gums or persistent bad breath, and attend regular dental check-ups so problems are treated before they become more serious.
Your next step is simple: book a dental check-up if you have not had one recently, then review your brushing, interdental cleaning, sugar intake, and smoking habits this week.