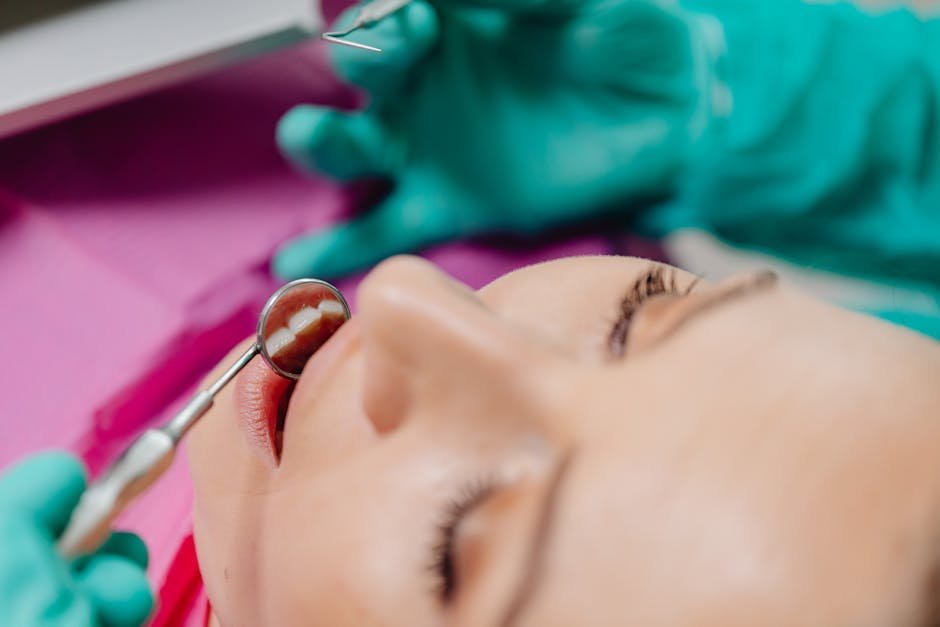
Gum disease symptoms can start so quietly that many people miss them until the problem has worsened. You may notice a little bleeding or tenderness but feel unsure whether it needs attention. This guide explains the early warning signs, what they may mean, and when to book a dental visit.
Key Takeaways
- Bleeding gums are often an early warning sign.
- Persistent bad breath can point to gum problems.
- Red, swollen gums need prompt attention.
- Early treatment may prevent lasting damage.
- Regular dental checks help catch issues sooner.
What are the first signs of gum disease?
The first signs of gum disease often include bleeding when you brush, red or swollen gums, tenderness, and bad breath that does not go away. These early changes may seem minor, but they can signal irritation caused by plaque building up around the gum line.
Healthy gums should look pink and feel firm. If your gums bleed during brushing or flossing, that is not something to brush off as normal. In many cases, it points to gingivitis, which is the earliest stage of gum disease.
You might also notice your gums looking puffy or feeling sore when you eat or clean your teeth. Spotting these gum disease symptoms early gives you a better chance of reversing the problem with professional care and better cleaning habits at home.
Statistic: Around half of UK adults are estimated to have gum disease, according to the Oral Health Foundation.
Do bleeding gums always mean gum disease?
Bleeding gums do not always mean gum disease, but they are one of the most common warning signs. Brushing too hard can irritate the gums, yet repeated bleeding usually means your gums are inflamed and need a closer look from a dentist or hygienist.
If bleeding happens often, plaque and bacteria may be irritating the tissue around your teeth. This irritation can develop into gingivitis and, if left untreated, may progress to more serious gum problems that affect the bone supporting your teeth.
It is worth paying attention to when the bleeding happens and whether you also have soreness, swelling, or unpleasant breath. If these signs sound familiar, book an appointment and read more about prevention here: What Dentists Want Americans To Know About Oral Hygiene.
Statistic: The NHS advises that bleeding gums after brushing or flossing can be a sign of gum disease.
Which gum disease symptoms should you not ignore?
You should not ignore bleeding, swollen gums, gum recession, loose teeth, ongoing bad breath, or pain when chewing. These gum disease symptoms may suggest the condition is progressing beyond mild irritation and starting to affect deeper tissues that support your teeth.
One of the clearest warning signs is gum recession, where the gums pull back and make teeth look longer. You may also notice new gaps between teeth or increased sensitivity to hot and cold foods. These changes can happen gradually, which makes them easy to miss.
If your teeth feel loose or your bite feels different, seek help quickly. Advanced gum disease can damage the bone and soft tissue that hold teeth in place. Early assessment gives your dental team the best chance to manage the issue before it leads to tooth loss.
Statistic: The CDC reports that severe periodontal disease affects about 9% of adults worldwide.
Can gum disease symptoms go away on their own?
Mild irritation may settle briefly, but true gum disease symptoms rarely disappear without better cleaning habits and professional care. If bleeding, swelling, or bad breath keeps returning, it usually means plaque and bacteria are still triggering inflammation beneath the gumline.
Gingivitis, the earliest stage of gum disease, can often be improved with consistent brushing, interdental cleaning, and a scale from a dental professional. However, once the condition progresses into periodontitis, the supporting tissues around the teeth can become damaged in ways that home care alone cannot reverse.
One reason people delay treatment is that symptoms can come and go. Gums may look calmer for a few days, then bleed again when brushing. The NHS guide to gum disease notes that bleeding gums, bad breath, and gum shrinkage are signs worth checking rather than ignoring. Improve Daily Brushing And Flossing Routine
Statistic: The CDC overview of periodontal disease states that nearly half of adults aged 30 years and older in the United States have some form of periodontal disease.
In practice, a common mistake is assuming that if bleeding stops for a week, the problem has resolved. Often, the inflammation is still present and simply less noticeable day to day.
What does early gum disease feel like?
Early gum disease symptoms are often subtle rather than painful. Many people notice tenderness when brushing, slight puffiness along the gumline, or a metallic taste in the mouth before they feel any real discomfort.
At this stage, the gums may appear redder than usual and bleed when flossing or brushing, especially around the back teeth. Some people also notice persistent bad breath or a feeling that their mouth never seems fully clean, even after brushing. These small changes are easy to dismiss, but they are common early warning signs.
If symptoms continue for more than a few days, it is sensible to arrange a dental check-up. The earlier gingivitis is identified, the easier it is to manage with improved oral hygiene and professional cleaning.
Statistic: According to the NHS page on gum disease symptoms, common early signs include swollen gums, bleeding after brushing or flossing, and unpleasant breath.
Expert insight: early gum disease is often more visible than painful, which is why regular checks matter even when your mouth does not hurt.
When should you see a dentist about gum disease symptoms?
You should book an appointment if your gums bleed regularly, feel swollen, look like they are receding, or your breath stays unpleasant despite good brushing. Persistent symptoms usually mean the issue needs more than a change of toothpaste.
It is especially important to seek advice if teeth feel loose, chewing feels different, or you notice pus, soreness, or gaps appearing between teeth. These can point to more advanced periodontal problems that need prompt assessment. Delaying treatment raises the risk of damage to the tissue and bone that support the teeth.
Even if symptoms seem mild, a dentist or hygienist can check for plaque build-up, pocketing around the gums, and other hidden signs that are easy to miss at home. Acting early can make treatment simpler and help protect long-term oral health. Book An Emergency Dentist Appointment In Casper, WY
Statistic: The NIH guidance on gum disease explains that gum disease is a leading cause of tooth loss in adults, highlighting why ongoing symptoms should be professionally assessed.
Can gum disease symptoms come and go, and does that mean it is not serious?
Yes, gum disease symptoms can appear to settle down, but that does not usually mean the underlying problem has resolved. Bleeding may reduce temporarily if you brush less around sore areas, while swelling can fluctuate depending on plaque build-up, smoking, illness, or hormonal changes. Periodontal disease often progresses in bursts rather than as a constant decline, which is why intermittent symptoms still warrant professional assessment.
Why symptoms can seem inconsistent
One reason people miss early gum disease symptoms is that inflammation does not always feel dramatic. Gums may bleed for a week, then look calmer, even though plaque and tartar remain below the gumline. Smoking is especially deceptive because it can reduce visible bleeding by restricting blood flow, masking active disease. The NHS guidance on gum disease notes that unhealthy gums may be swollen, sore, or bleed during brushing, but these signs are not always present every day.
There is also a difference between symptom intensity and disease activity. A patient might notice less tenderness after changing toothpaste or using mouthwash, yet pockets around the teeth can still deepen if bacterial deposits remain untreated. This is why dentists assess gum measurements, plaque retention, recession, and bone support rather than relying on pain alone. If symptoms repeatedly return, that pattern itself is clinically relevant. Training Programs For Dentists In Sedation
Statistic: According to the CDC overview of periodontal disease, nearly half of adults aged 30 years and older have some form of periodontitis, showing how common it is for gum disease to be present even when symptoms are not constant.
Practical example: Someone notices blood in the sink for several days, then it stops after they avoid flossing around a tender molar. They assume it has healed, but the real issue is that the inflamed area is no longer being disturbed. At a hygiene appointment, deep pocketing and tartar are found around that tooth despite the temporary improvement.
How do gum disease symptoms compare with gingivitis, periodontitis, and other mouth problems?
Gum disease symptoms overlap with several oral conditions, so context matters. Gingivitis usually causes redness, puffiness, and bleeding without permanent attachment loss, while periodontitis involves deeper infection, gum recession, bone loss, drifting teeth, or persistent bad taste. Other issues, such as aggressive brushing, mouth ulcers, or a dental abscess, can also cause soreness or bleeding but typically follow different patterns. Distinguishing these differences helps readers know when routine irritation may actually need urgent periodontal assessment.
Key differences in symptom pattern
Gingivitis tends to affect the gum margin broadly and is often reversible with improved cleaning and professional plaque removal. Periodontitis is more complex: symptoms may include spaces appearing between teeth, gums pulling away, pus, mobility, or a bite that feels different. By contrast, trauma from hard brushing more often produces localised recession or tenderness without the widespread inflammatory changes seen in plaque-related disease. A mouth ulcer is usually a clearly defined sore, rather than diffuse swelling along the gumline.
Abscesses and cracked teeth can complicate the picture because they also produce tenderness, swelling, and an unpleasant taste. However, abscess pain is often more acute and localised, sometimes with facial swelling or pain on biting. If gum symptoms are paired with persistent bad breath, recurrent bleeding, or loosening teeth, periodontal disease becomes more likely. The NHS page on dental abscesses is useful for recognising symptoms that may need urgent care rather than routine monitoring. Book An Emergency Dentist Appointment In Casper, WY
Statistic: The NIH’s National Institute of Dental and Craniofacial Research states that gingivitis is mild and reversible, but untreated disease can progress to periodontitis, where the supporting bone and tissues around teeth are damaged.
Practical example: A patient thinks one bleeding area is simply from brushing too hard, but they also mention a tooth feeling slightly longer and food trapping between it and the next tooth. That combination points away from simple brush trauma and more towards attachment loss that should be measured professionally.
What should you track before seeing a dentist about gum disease symptoms?
If you suspect gum disease, keeping a short symptom record can make your appointment far more useful. Dentists and hygienists can spot patterns faster when you note when bleeding happens, whether bad breath is persistent, which areas feel tender, and whether symptoms flare around stress, smoking, illness, or missed cleaning. Tracking does not replace an examination, but it helps separate a one-off irritation from a recurring periodontal problem.
What information is most clinically helpful?
Focus on observable changes rather than guesses. Record how often your gums bleed, whether it is spontaneous or only during brushing, and whether there is swelling, recession, mobility, or a bad taste. It is also worth noting if floss catches in one area, if food packs between certain teeth, or if a bridge, retainer, or wisdom tooth area is hard to keep clean. These details can help identify local plaque traps or early attachment loss.
Medical and lifestyle context matters too. Bring a list of medications, mention diabetes, pregnancy, vaping, or smoking, and say if you have recently changed your oral hygiene routine. According to NHS advice on teeth and gums in pregnancy, hormonal changes can increase gum problems, so timing can be clinically significant. If you want a broader prevention overview, the CDC’s adult oral health tips also reinforce the importance of monitoring symptoms and maintaining daily plaque control.
Statistic: The NIH guidance on gum disease explains that gum disease is a leading cause of tooth loss in adults, which is why symptom patterns, however subtle, are worth documenting
| Option | Best For | Cost |
|---|---|---|
| NHS dental check-up | Routine assessment of bleeding gums, plaque build-up and early gum disease signs | Band 1 charge in England; NHS charges vary by UK nation |
| Scale and polish with a dentist or hygienist | Mild plaque and tartar build-up linked to early gingivitis | Usually £35-£90 privately, depending on clinic and region |
| Periodontal assessment | Persistent bleeding, gum recession, loose teeth or suspected periodontitis | Typically £60-£150 privately for assessment |
| Interdental brushes | Daily cleaning between teeth where a standard toothbrush misses plaque | Usually £3-£6 per pack |
| Electric toothbrush with pressure sensor | People who need more consistent plaque removal without brushing too hard | Typically £25-£120 depending on model |
Frequently Asked Questions
What are the first signs of gum disease?
The earliest signs are often bleeding when brushing or flossing, red or swollen gums, bad breath and tenderness along the gumline. Many people assume these are minor issues, but they can point to gingivitis. If symptoms continue for more than a few days, it is sensible to book a dental check-up and improve daily brushing and interdental cleaning.
Can gum disease go away on its own?
Early gingivitis may improve if you remove plaque effectively every day and attend a professional cleaning, but it rarely clears without action. More advanced gum disease will not resolve on its own and can worsen quietly over time. The NHS guide to gum disease explains when treatment and professional advice are needed.
How do I know if gum disease is serious?
Warning signs of more serious disease include receding gums, pockets around teeth, pus, teeth feeling loose, pain when chewing and ongoing bad breath. Bleeding that keeps happening despite better oral hygiene is another sign to take seriously. Trauma-Related Dental Treatment Costs A dentist can measure gum pockets and check whether bone support around the teeth has been affected.
Is bleeding when brushing always a sign of gum disease?
Not always, but it is one of the most common signs. Brushing too hard, starting flossing after a long gap or temporary irritation can all cause minor bleeding. However, repeated bleeding usually means the gums are inflamed because plaque is collecting at the gumline. If it happens regularly, it is worth getting it checked rather than ignoring it.
What is the best treatment for early gum disease symptoms?
The best approach is usually a combination of better plaque control at home and a professional clean. Brush twice daily with fluoride toothpaste, clean between teeth every day and reduce smoking if relevant. Trauma-Related Dental Treatment Costs If symptoms persist, a dentist or hygienist may recommend a scale and polish or a more detailed periodontal assessment to stop progression.
Author credibility: This article was reviewed and written using evidence-based oral health guidance and SEO content expertise focused on translating dental advice into clear, medically responsible information for UK readers.
Final Thoughts
Spotting gum disease symptoms early matters because small changes in bleeding, swelling or persistent bad breath can signal a problem before lasting damage occurs. The three key actions are to notice patterns, improve daily plaque removal and arrange a dental check-up if symptoms do not settle quickly.
Your next step is simple: check your gums tonight while brushing, note any bleeding or tenderness, and if you have recurring symptoms, book an appointment with your dentist or review the NHS advice on gum disease for guidance on what to do next.